Callus Causes: Why Hard Skin Forms on Your Feet
- Lamar| The Foot Aftercare Institute
- Mar 3
- 5 min read
Updated: Mar 28
Calluses are a common foot issue that many people encounter, often without a second thought. However, understanding what causes these hard skin formations is crucial to managing and preventing them effectively.

What Is a Callus?
A callus is an area of thickened skin that develops as a protective response to repeated pressure or friction. Unlike corns, calluses are broader, less defined, and usually less painful. They most commonly appear on:
The heel
The ball of the foot
The side of the big toe
Over surgical scars
To get a deeper understanding of the differences between calluses and corns, check out Foot Corn Types Explained.
What Causes Calluses?
Calluses form when your skin tries to protect itself from repeated stress. Here are the main causes that contribute to their development:
Repeated Friction
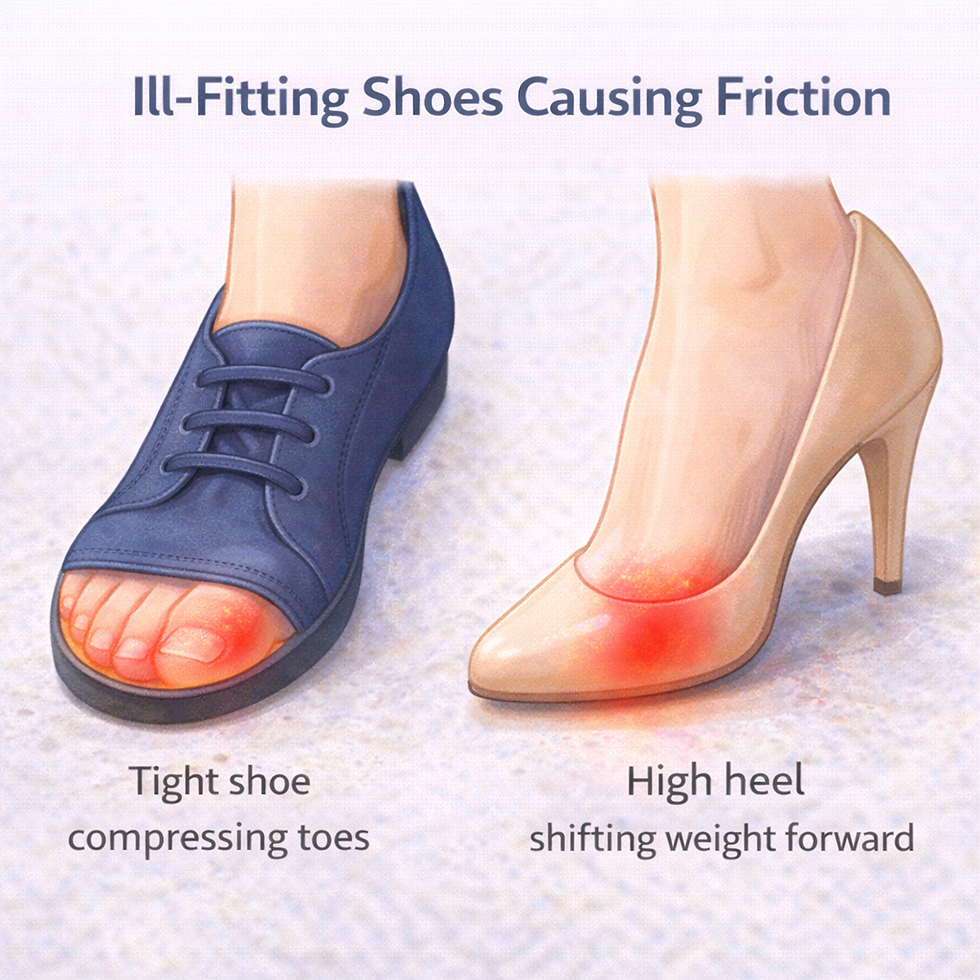
One of the primary causes of callus formation is repeated friction. Tight shoes, rough seams, or prolonged rubbing create skin irritation.
The body responds to this irritation by thickening the outer layer of skin.
Common triggers include:
Narrow footwear
High heels
Hard flooring surfaces
Long walking distances
As pressure continues, the callus thickens and becomes more pronounced.
Pressure from Abnormal Foot Mechanics
Your walking pattern significantly affects where pressure is distributed across your feet. People with conditions such as flat feet, high arches, overpronation, or structural toe differences often develop calluses in specific areas due to abnormal pressure zones.
To understand which foot type you might have, learn more in Foot Types and Toe Shapes Explained.
Scar Tissue After Surgery
Scar tissue behaves differently from normal skin and can create uneven pressure zones. When thick skin forms over a surgical site, it may resemble a callus but actually sits atop scar tissue.
It’s essential to distinguish between the two to avoid mismanagement. For more insight, see Callus Over Scar: Why It Happens & How to Fix It Safely.
Poor Footwear Support
Worn-out shoes or those with thin soles can increase impact forces on your feet. Without adequate cushioning, the skin is subjected to repeated mechanical stress, which triggers thickening to protect itself.
Adding supportive insoles might help redistribute pressure and mitigate the risk of calluses.

Barefoot Walking on Hard Surfaces
Walking barefoot on hard surfaces such as tile or concrete increases micro-pressure with each step.
Over time, this consistent impact encourages protective thickening of the skin, leading to callus formation.
Untreated Dry Skin
Dry skin is not only uncomfortable but also more likely to crack and thicken unevenly. Applying appropriate moisturisers regularly can help maintain skin hydration and reduce excess build-up.
For guidance on using moisturisers, see How to Use Urea Cream and Silicone Gel Properly.
Are Calluses Always a Problem?
Not necessarily. Mild calluses often act as a protective barrier against friction and pressure. However, they can become problematic when they meet specific criteria:
They crack or bleed
They cause pain
They turn yellow and dense
They show signs of redness or swelling
They appear in people with diabetes
It's crucial to look out for warning signs. To learn more about complications, read Infected Foot Callus: Symptoms, Treatment & When to See a Podiatrist. If you have diabetes, it's wise to review Diabetic Foot: Warning Signs & Prevention.

Callus vs Corn: What’s the Difference?
Understanding the difference between calluses and corns is essential for proper foot care.
Calluses are larger, diffuse, and usually painless.
Corns are smaller, typically have a central core, and are often painful.

How to Prevent Calluses
Prevention is often the best strategy for calluses. Focus on reducing the pressure and friction that lead to their development.
Here are actionable steps to consider:
Wear properly fitted shoes: Ensure your shoes have enough room and aren't too tight.
Use cushioned insoles: These can provide additional support and reduce pressure on sensitive areas.
Regular gentle filing: Use a pumice stone or foot file to keep calluses at bay.
Daily moisturising: Applying lotion can prevent dry skin, reducing the risk of calluses.
Monitor pressure points: Be aware of areas on your feet that endure frequent pressure and take steps to mitigate it.
For overall maintenance, see Healthy Feet: What Do Healthy Feet Look Like?.
When should you seek out a podiatrist?
You should seek professional care from a podiatrist if:
The callus is painful
It keeps returning despite home treatment
You notice reduced sensation in your feet
You observe signs of infection
You’re unsure whether it’s a callus or scar tissue
For additional guidance, check out When to See a Podiatrist for Foot Problems.

Further Reading from The Foot Aftercare Institute:
Explore more expert tips and foot care guides to support your skin health recovery
Callus Over scar: Why it Happens& How to Fix It
Discover why thickened skin can form over surgical scars and how to manage it safely at home.
Not sure if it's a corn or a callus? Learn the key differences and how to identify each correctly.
Infected Foot Callus: Symptoms, Treatment & When to See a Podiatrist
Understand the warning signs of infection and when thickened skin becomes a medical concern.
Chronic dryness can worsen thickened skin. Learn how moisture loss contributes to rough, hardened areas.
How to Use Urea Cream Properly
Step-by-step guidance on safely softening thickened skin without causing irritation or over-exfoliation
Know when self-care isn't enough and professional treatment is the safest option
Final Thoughts on Callus Causes
Understanding the causes of calluses is an excellent first step in managing them effectively.
By taking preventive measures and seeking professional advice when necessary, you can maintain the health of your feet and minimise the discomfort associated with calluses.
Remember, while they often serve a protective purpose, severe or painful calluses shouldn't be ignored.
Taking proactive steps will not only enhance your foot health but also improve your overall quality of life.



Comments